 The volume that enters the lung per minute is known as minute ventilation (VE). There are two equations needed to calculate the volume that enters the lungs and the volume that reaches the alveoli. Ventilation is the manner by which air enters the lungs. One can see an increase in the value of physiologic dead space in lung disease states where the diffusion membrane of alveoli does not function properly or when there are ventilation/perfusion mismatch defects. Therefore, physiologic dead space is equivalent to anatomical. In a healthy adult, alveolar dead space can be considered negligible. The respiratory zone is comprised of respiratory bronchioles, alveolar duct, alveolar sac, and alveoli. 
Physiologic or total dead space is equal to anatomic plus alveolar dead space which is the volume of air in the respiratory zone that does not take part in gas exchange. This volume is considered to be 30% of normal tidal volume (500 mL) therefore, the value of anatomic dead space is 150 mL. Anatomical dead space is represented by the volume of air that fills the conducting zone of respiration made up by the nose, trachea, and bronchi. The two types of dead space are anatomical dead space and physiologic dead space. The A-a gradient can be calculated by subtracting the alveolar partial pressure of oxygen, which is calculated using the alveolar gas equation, by the arterial partial pressure of oxygen, measured with arterial blood gas (ABG).Dead space represents the volume of ventilated air that does not participate in gas exchange. All three of these conditions can contribute to an increase in A-a gradient and cause hypoxemia. 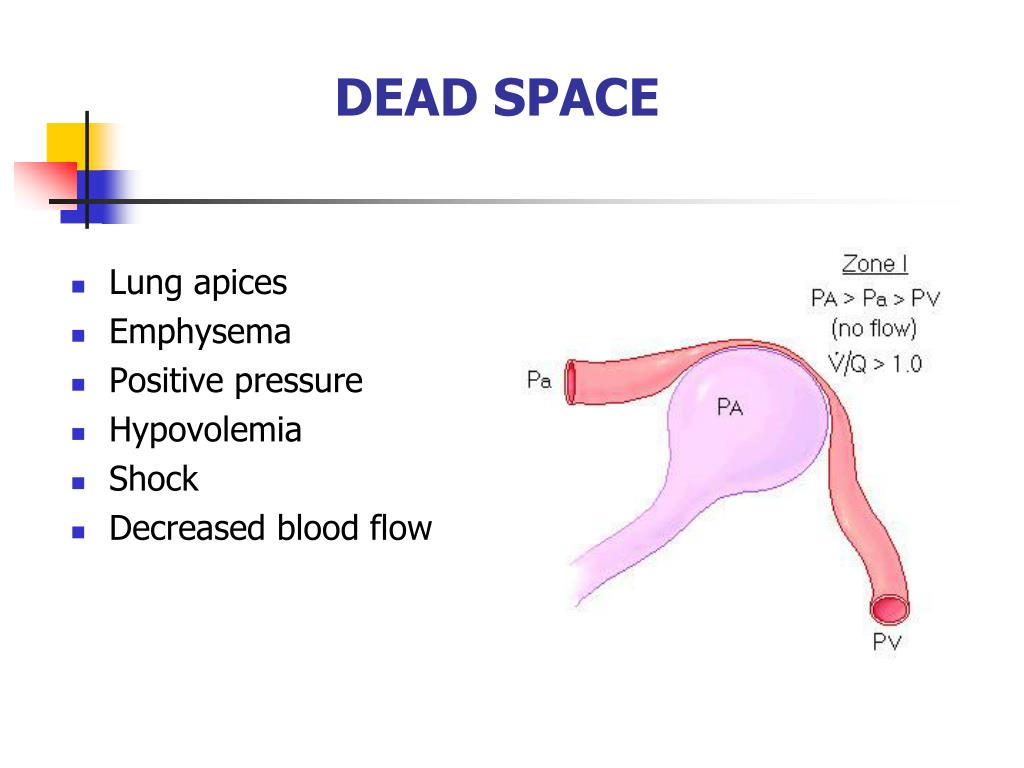
Diffusion problems can occur when the alveolar walls are fibrosed and oxygen cannot diffuse across the alveolar wall into the blood stream. High V/Q is also called dead space and low V/Q is called shunting. V/Q mismatch means a mismatch of ventilation to perfusion (V/Q) ratio and can represent either too little perfusion due to blood flow obstruction (high V/Q) or too little ventilation due to airway obstruction (low V/Q). An increase in A-a gradient can occur in hypoxemia and the causes include V/Q mismatch such as dead space or shunting and diffusion problems. The normal A-a gradient is 10 to 15 mmHg. 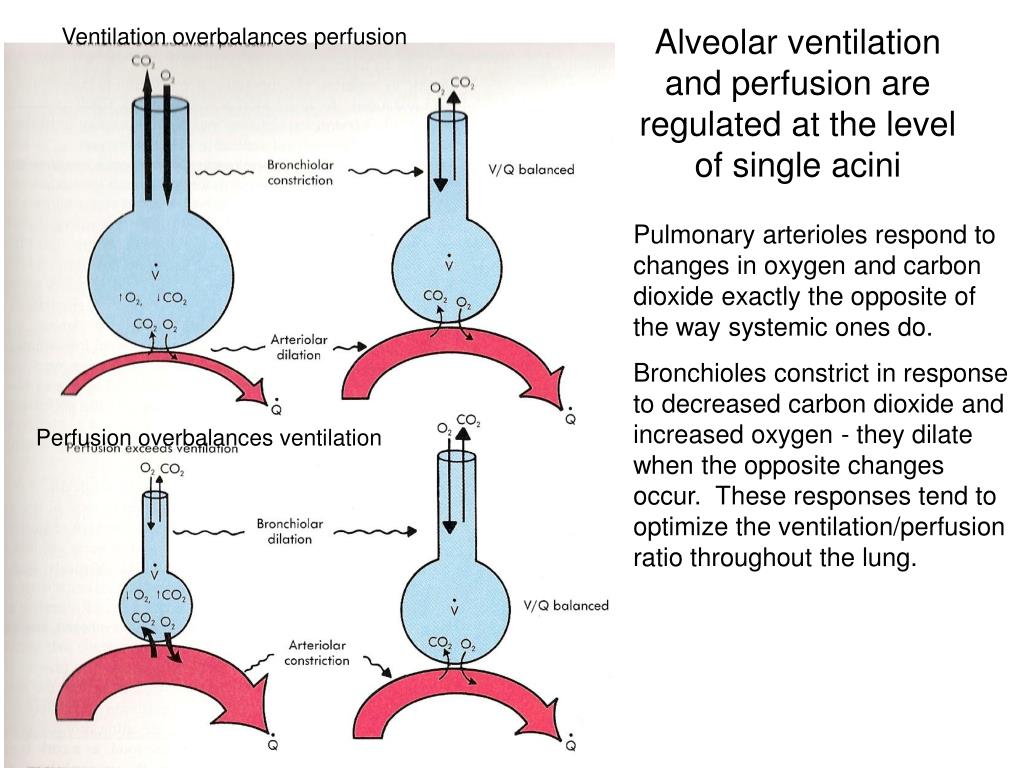
The A-a gradient represents the difference in partial pressure of oxygen between the alveoli and the arteries. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
